Black Fungus Infection In Covid Cases

What is Black fungus (Mucormycosis)?
Mucormycosis is commonly known as black fungus which is a rare condition but also a serious fungal infection. It is caused by a kind of fungi called mucoromycetes. This fungus is abundant in the environment all around us. In fact, this fungus affects the people having some health problems. In addition, it affects people taking medications that lower the body’s ability to fight against the germs. It usually affects the nose, sinuses, eye and brain to produce varying symptoms. It can also affect other parts such as lungs, stomach, intestines and skin.
How black fungus enters our body?
This black fungus spreads by its spores of molds entering through mucosal lining. Usually it comes through inhalation, eating contaminated food, or contact with open wounds. This fungus is common in soil, decomposing organic matter and animal manure. It does not transmit between the people.
Where these black fungi exist?
Mucormycetes is the group of fungi which cause mucormycosis (black fungus). These are present in the environment mostly in the soil and decaying organic matter like leaves, compost piles and animal dung. This fungus is more common in soil than in air. These fungi are mostly harmful but people with deficient immune systems suffer more often. The fungal spores can cause an infection in lungs or sinuses which can also spread to other parts of the body.
What are the symptoms of black fungus disease?
As other fungal infections black fungus disease can infect skin, cornea of eyes and deep layers of the skin, viscera or organ involvement, or as allergic reactions. In diabetic individual black fungus spreads rapidly and causes severe disease. As this fungus has a tendency to infect the air cavities like sinuses and lungs it causes serious infection of face, nose, eyes and brain. In severe cases it can spread through blood as well.
- Pain and redness around the eyes or nose.
- Fever
- Headache
- Coughing
- Runny nose
- One side facial swelling and pain
- Swollen
- Bulging eye
- Shortness of breath
- Bloody vomits
- Altered mental status
- Tissue death
| Sites of Infection | What can happen? | Complications |
| Skin | Abscesses, skin swelling and necrosis | Can spread to muscle, tendons & bones |
| Nose | Sinus pain, nasal congestion, fever, soft tissue swelling and headache | Ulcer or thrombosis of palate |
| Eye | Blurred vision or even complete loss of vision | Can spread to Brain |
| Brain | Altered consciousness, cranial neuropathies or cerebral abscesses | Highly fatal disease |
| Lungs | Fever and cough , pleuritic chest pain and dyspnea | Blood vomiting, severe lung disease |
| Gut | Abdominal pain, distention together with nausea and vomiting | Can spread to liver, spleen & kidneys |
Risk factors for black fungus infection:
Mucormycosis is a rare but also more common disease among people who are all having health problems and also who are all taking medicines for sickness. Certain groups of people are most common to get black fungus.
- Diabetes
- Cancer
- Organ transplant
- Stem cell transplant
- Neutropenia
- Long term corticosteroid use
- Injection drug use
- More iron in body
- Skin injury due to surgery, burns, wounds
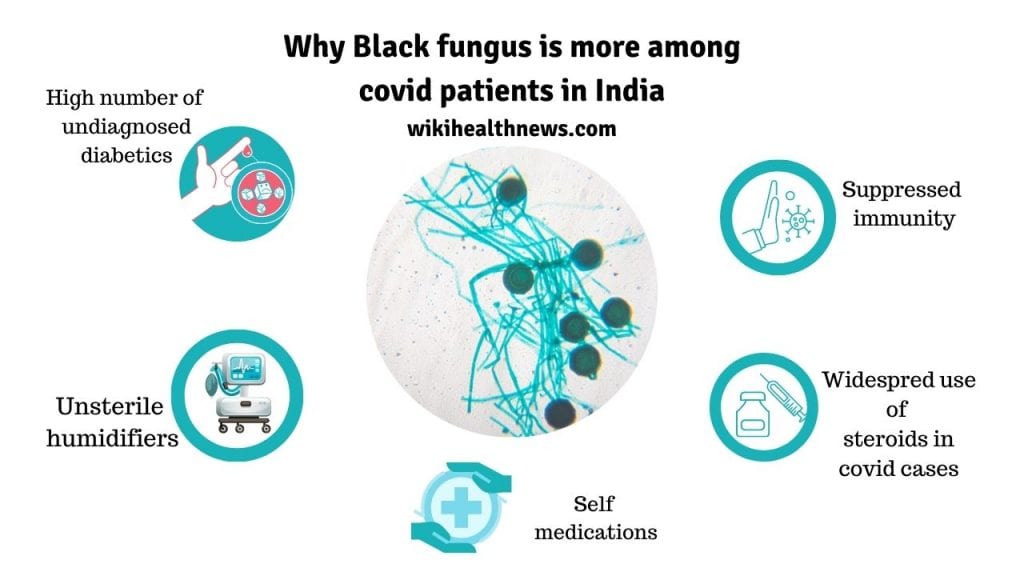
What are some causes of black fungus disease in COVID-19 patients?
Recently, many coronavirus patients, or those who have recently recovered from Covid-19 are diagnosed with black fungus disease. These cases are rising in countries like India which currently has 70% of black fungus disease of the world. Post covid cases with low immune systems most notably diabetics are the sufferers. At present around 12000 cases have been diagnosed in India.
Covid patients in ICU are also susceptible to this disease. It trasmits through the infected humidifiers to patients on oxygen support.
How does someone get mucormycosis?
People will get black fungus through contact with fungal spores in the environment. The infection spreads to lungs which occur after someone inhales the spores from the air. A skin infection which also occurs after the fungus enters the skin through scrape, burn, or kind of skin injection. From there it can spread to the eyes, potentially causing blindness, or the brain, causing headaches or seizures. Patients can acquire wound infection after surgery in hospital. Mucormycosis causes disfiguring of wounds. This mucormycosis dose not spread between people to people or animals.
Diagnosis of Mucormycosis
History, symptoms, physical examinations and some lab tests can help to diagnose this infection. Lungs tissue biopsy can show the fungus under microscope. Fungal culture from tissue of lungs are also specific. Imaging tests like CT, MRI scan of lungs, sinuses of different parts depending on the location can be done as well.
Prevention
- It is important to be safe from fungus or viral disease.
- Try to avoid places with a lot of dust places like construction or excavation sites. If you can’t avoid it then wear an N95 mask in public places.
- Avoid direct contact with contaminated water.
- Prevent activities that involve close contact with soil or dust
- Wear shoes, long pants, and long sleeved shirts when you are going outside.
- Use gloves when you are handling materials like soil, moss or manure.
- Avoid skin infection, keep clean skin, clean the skin injuries with soap and clean water.
- Use some antifungal medication.
- There is no vaccination to prevent from black fungus.
Treatment:
Mucormycosis is a serious infection which needs to be treated. The infection needs to be treated with prescription of antifungal medicine, like Amphotericin B, Posaconazole or Isavuconazole. Other medicines are Fluconazole, Voriconazole and Echinocandins will not work against this black fungus. Often mucormycosis requires surgery to cut away the infected tissues. These are injections which has to be given directly through veins.
Read more